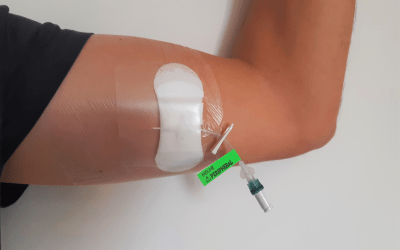
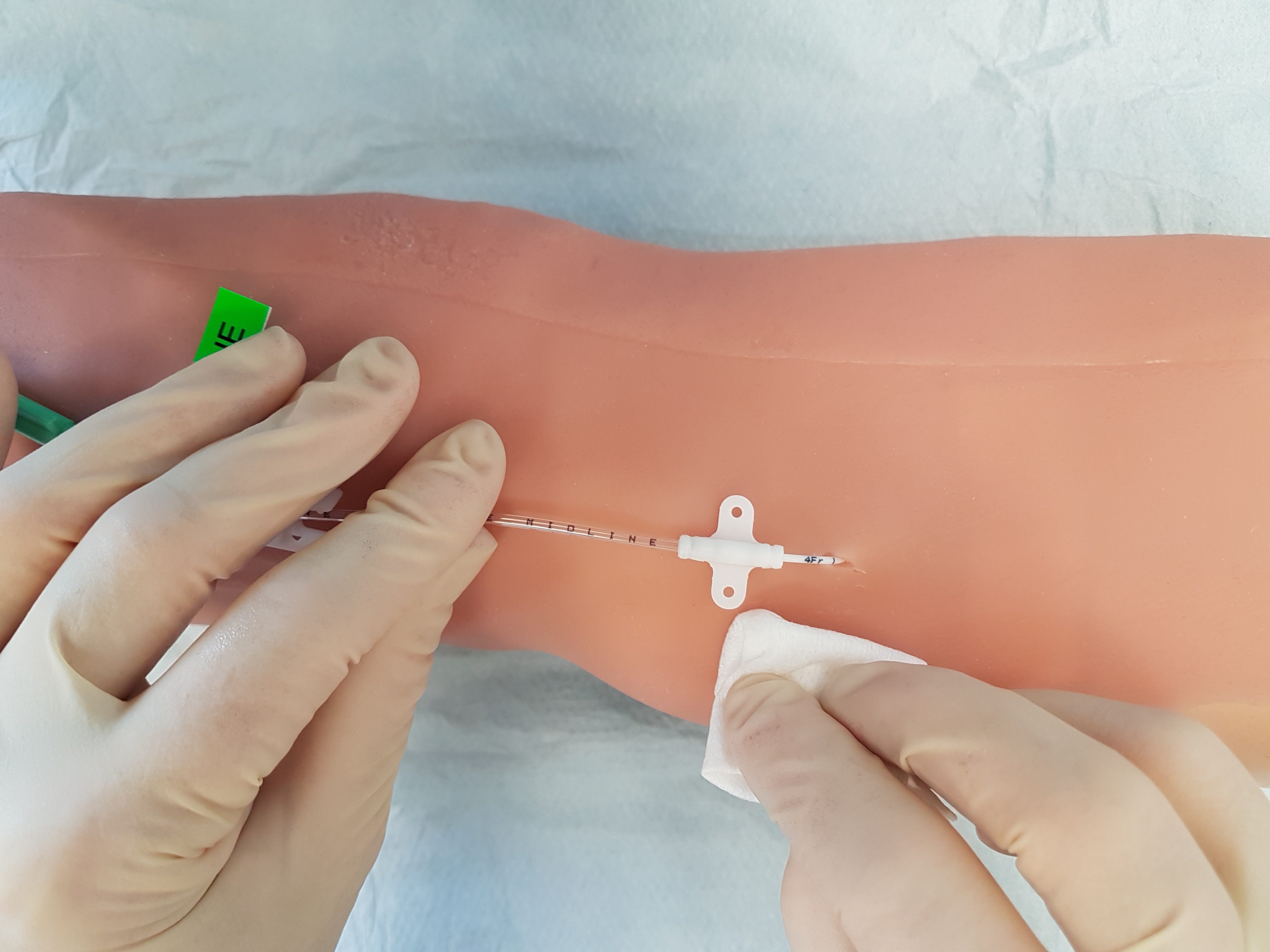
Acute Cardiac Care Unit, Crosshouse Hospital, NHS Ayrshire & Arran, Scotland Within cardiology, there is a cohort of patients who require prolonged IV access, such as those with...
Midlines
You can find all the articles linked to Midlines in this page.
Everything you need to know about tunnelling in midlines
In ultrasound-guided procedures, it is possible that an ideal vein isn't found in the optimal catheter exit zone. When confronted with the decision between "immediate placement of a line out of...
5 key advantages of midlines you should know of
Short Peripheral Intravenous Catheters (SPIVCs) are commonly used as default vascular access devices by practicians around the world for short and midterm therapies. However, they can be a problem...
Short Peripheral Intravenous Catheters (SPIVC) vs Extended Dwell Catheters (EDC)
Introduction The aim of this article is to describe and discuss some differences between the short peripheral intravenous catheter (SPIVC) and the long peripheral intravenous catheter (LPIVC)...
Inadequate care in midlines: 5 complications to know
Intravenous therapy is a usual treatment for hospitalized patients and increasingly, for those who are at home. The administration of drugs can give rise to problems such as phlebitis and extravasation among others, which can force us to use various peripheral routes. Over time, different devices have emerged, including midlines…
Midline catheter: placement and maintenance protocol
The midline catheter growth has been exponential since it is a resource that allows a notable improvement in the management of vascular access for medium-term treatments compatible with peripheral perfusion…
Peripheral vascular access of elderly patients: what are the available options?
In this article, we will see what the impact of elderly patients is on hospitals and how peripheral vascular access can be managed when such patients require intravenous treatment.
The varying terminology surrounding Midline Catheters
Vascular Access Devices (VADs) are divided into two basic groupings, peripheral and central. The group delineation is determined, primarily, by the catheter tip termination position, rather that the insertion site. Peripheral catheter tips remain in the periphery, terminate distal to the subclavian or femoral vein, and are optimal for intravenous medications that are peripherally compatible.
Midline Catheter at home
This pandemic has confirmed a reality for us: hospitals are for acute patients. Although this is not new, we are now able to put it into action: now more than ever our home is our shelter. Home health care, specifically in the field of vascular access, IS feasible.
Short Peripheral Catheter: Four Common Problems
As nurses, do we know how invasive it is and what the consequences are of inserting a short peripheral catheter into a vein? In May/June 2015, the “Journal of Infusion Nursing” dedicated an article...
Midline Catheters in Paediatrics
The characteristics that define midline catheters are well established. However, in recent years a new group of peripheral vascular access devices has appeared on the market: long peripheral catheters (long peripheral IV catheters), also known as “mini-midlines”. The characteristics of both devices are summarised in Figures 1 and 2.